15.10.15
Two-thirds of hospitals are inadequate and variation in care is ‘shocking’
Two-thirds of NHS hospitals are offering substandard care or failing altogether, while providers across the social care, mental health and primary care sectors raised grave concerns in regards to varying safety and staffing levels.
The CQC’s annual report into state of care in England confirmed the challenging times that providers are facing, with all being asked to do more with less as the health service and local authorities receive insufficient funding to meet growing demand.
The investigator found that both the NHS and the social care sectors had to cope with increasing pressures despite budgets seeing smaller increases than before.
As a result, the variation in quality of care, particularly in regards to safety, was of primary concern – with some people receiving unacceptable care and nearly 10% of all sectors being rated as inadequate.
Examples of intense concern in inadequate providers included A&E patients being kept on trolleys overnight in a portable unit without proper nursing assessments, medicine being given without appropriate patient identification, or GP surgery staff not having basic life support training.
Regulators also found that medication was not administered properly in care homes and, in nursing homes, there was an overpowering smell of urine and mould on the walls.
CQC’s chief executive, David Behan, said: “A key concern has been the safety of the care – a failure to learn when things go wrong, or not having the right number of staff in place with the right skills.
“The variation in care that we have observed is not just about the money. Good leaders are what make the difference – leaders who engage staff and people who use services and create a culture of continuous quality improvement. What is very clear is that isolated working and incremental changes are not going to be enough to meet the challenges ahead.”
Health secretary Jeremy Hunt agreed that the level of variation in care is unacceptable, but recognised that there were some excellent examples of high quality care countrywide.
He said: “That’s exactly why we set up CQC’s independent inspection regime which shines a light on poor care to drive up standards.”
But Heidi Alexander MP, shadow health secretary, said Hunt cannot keep ignoring these serious warnings about unsafe and understaffed hospitals.
More information on each sector below.
Hospitals
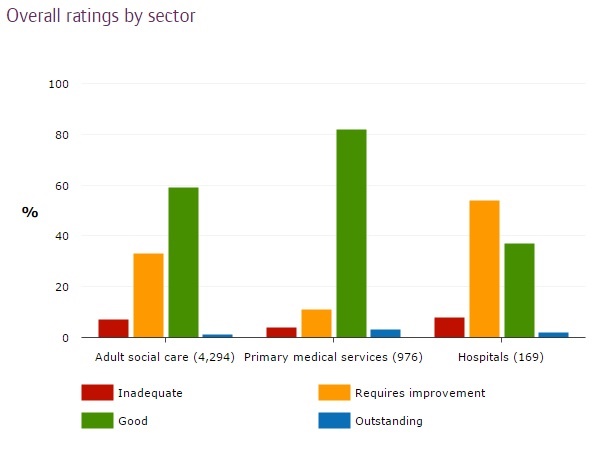
Hospitals formed the only sector in the study where most providers were rated as inadequate or failing (as opposed to good or outstanding). Nearly two-thirds (62%) of all hospitals were failing, while all contributed to a concerning variation in standards of care across the board.
The CQC also reported concerns about the leadership and culture in many trusts, but highlighted patient safety as topping the list of grievances – primarily driven by low staffing levels and skill mix.
And while 35% were rated as either good or outstanding, the inspection body said that aggregated ratings at trust level mask the substantial variation amongst individual hospitals, as well as variation of individual core services within a single hospital.
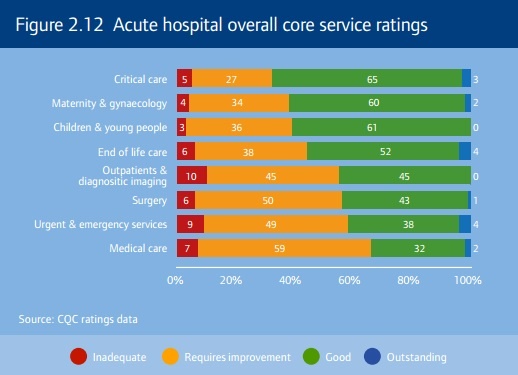
In ‘inadequate’ trusts, there was a culture where frontline staff were unable to raise concerns about patient care, and a history of the leadership team taking false assurance from inadequate information. They also displayed poor leadership and teamwork in clinical teams and weak relationships with external stakeholders.
The CQC also reported poor patient flow, inappropriate admissions and delayed discharges, alongside a general failure to carry out basic safety checks and day-to-day crisis management rather than long-term planning.
Rob Webster, chief executive of the NHS Confederation, said that times are the toughest of a generation, but that other significant conclusions must also be drawn from the report apart.
He said: “No organisation is an island, so we need a fundamental shift in the way we regulate care. We’ve seen some progress but more is needed. A&E performance, for example, is a function of community support, social care and the local people as much as hospital staffing. Regulators should look at health and care systems, not just individual organisations.
“Leaders must be supported to deliver safe patient care and to transform the way we deliver care. This must be accompanied by an end to the ‘toxic’ environment that is creating a revolving door of NHS leadership, which is bad for the health service, and bad for patients. The CQC have a role to play here, as do NHS England and NHS Improvement.”
Similarly, Dr Peter Lachman, clinical lead for the SAFE programme at the Royal College of Paediatrics and Child Health, said: “Crucially, when things go wrong, we need to learn why and determine how we get things right today, tomorrow and in the future. There needs to be a continuous study environment which enables us to do this, but we need to do this in real time – not months after an incident occurred.
“There is a lot of good work that is going on in hospitals. It is this we need to learn from to ensure that patients, no matter whether they are being treated in the country, have safe care.”
Adult social care
The commission deemed it a key concern that 10% of adult social care providers were rated as inadequate for safety, also caused primarily by low staffing levels and poor medicine management.
In challenging times where local authorities were seeing their budgets slashed, the CQC found that 7% of social care providers were failing, unable to deal with the changing complex needs of an ageing population.
In addition to failing providers, 33% of the sector still required improvement.
But despite this, the social care sector was ahead of hospitals in terms of ratings, with 60% of providers being rated as either good or outstanding compared to just half of that within trusts.
Mental health
Although most mental health trusts were rated as good, 34% were still failing or required improvement.
Despite excellent examples of leadership, some boards were unaware of whether their decisions were having any impact on frontline services.
The safety of care environments in mental health wards was the CQC’s primary concern, alongside bed shortages still leading to people being forced hundreds of miles away from their families to receive care.
The investigator also reiterated what it had previously found: those with mental health needs, especially within minority ethnic groups, were less likely to report positive experiences in health and social care settings.
Primary care
The investigator was astounded at the very poor care provided by 4% of general practices rated as inadequate, despite most GP practices and out-of-hours services being rated positively.
Some examples were so shocking that the CQC had to shut down registrations where care was too poor, and where there was a real concern for patient safety. This means the provider could not legally continue to provide a service and NHS England worked on alternative arrangements for patients.
It also revealed a need for GP practices to review access to medical advice and treatment to ensure they are in line with patients’ needs, along with the system-wide call to improve leadership, medicines management and learn from mistakes.
According to the CQC, practices can deliver a better quality of care when they are sharing learning and providing joined-up care through multi-professional networks. Single practices often resulted in a lack of communication and engagement with staff and patients and an environment not sufficiently open and transparent.
It also recorded mounting pressure from a rise in the number of patients registered with a GP and the number of unfilled GP posts. Fewer people are entering the profession, 34% are considering retirement in the next five years and the sector faces pressures to ensure the current workforce can meet growing demand.
Responding to this, the chair of the Royal College of GPs, Dr Maureen Baker, said: “Where practices are struggling to meet quality standards, it is often due to factors beyond their control, such as a lack of funding, significant increases in patient consultations and difficulties in trying to recruit sufficient GPs to meet patients’ needs.
“The biggest threat to patient safety is tired doctors and GPs worn out as result of working flat out to manage rocketing patient numbers and ever-dwindling resources.”