12.08.15
Two-thirds of trusts spend at least double their agency forecast
The growing use of agency staff by trusts in the NHS has reached epidemic proportions and forced the government to clamp down on the practice. NHE’s David Stevenson investigates the scale of the problem.
Nearly 70% of NHS trusts and foundation trusts spent at least double what they had budgeted on agency staff in the last financial year, an NHE investigation has revealed.
Monitor and the NHS Trust Development Authority (TDA) – which are to be merged as ‘NHS Improvement’ – have already revealed that NHS trusts and FTs spent more than £3.3bn on agency staff in the last 12 months.
NHE sent freedom of information (FoI) requests to all of the trusts who sent copies of their draft accounts to the two organisations. Of our 240 requests, we got 176 replies – a return rate of 72%.
The 176 respondents included community, ambulance, mental health and acute trusts and FTs. Only 111 set a budget for or forecasted their agency spend for 2014-15. Of the 75 trusts that did not plan for their agency spend, one of the most common answers was that “we budget on the assumption that all roles are substantive roles – therefore we do not set specific temporary staffing budgets”.
However, of those that did set budgets, just under 70% (77 out of 111) spent at least double the amount they had planned to.
The worst underestimate was at Yorkshire Ambulance Service NHS Trust (YAS), which spent £3.72m on agency staff – 32 times more than the £110,099 forecast. That forecast was just for admin and clerical temps, when in fact it spent £2.08m on this class of workers and a further £1.1m on agency nurses – when it had not forecast spending anything at all on those.
However, YAS’s spending on agency staff as a proportion of its £161m total staffing bill was only 2.31% – far lower than most of the trusts who replied to our requests.
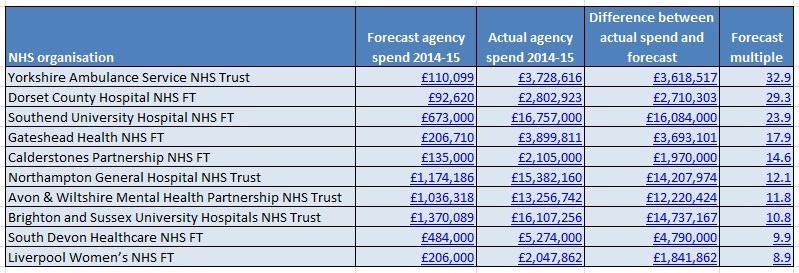
Dorset County Hospital NHS FT spent 29 times what it had budgeted on agencies. It had planned to spend only £92,620 on all agency staff (£53,333 on medical & dental staff and £39,287 on nursing & midwifery) but ended up spending £2.8m, of which £1.08m was for nurses and midwives.
Dorset had, though, budgeted to spend £2.95m on bank nursing and midwifery staff, but this fell to £1.57m in the annual accounts. And it looks as though the agency staff were used to offset this.
While these two trusts certainly didn’t have the largest agency staffing bill of those who responded to our FoI requests, it was striking how much they had overspent in comparison to what they had forecast.
Southend University Hospital NHS FT spent £173.9m on its staffing bill, having originally held £673,000 (or 0.3% of its staff budget) for areas where it knew specific cover would be required.
Adrian Buggle, the hospital’s deputy director of finance, said: “Our forecast year-end spend on agency cover, prepared in September 2014, was £15.9m and our total year-end spend was £16.7m. The £673,000 stated in the FoI response was funding held for areas where we knew there would be specific cover required, and was not a forecast of agency spend for the entire year.
“Much of our agency cover expenditure is funded from vacant posts that we have worked to fill during the year. This is not recorded as funds set aside specifically for agency cover, as the money covers substantive posts when they are filled. In order to mitigate agency fees, an additional £1.278m premium was available in reserves as well as funding from vacant posts within the trust.”
Southend spent just shy of 10% of its entire staffing budget on agency workers, primarily medical (£8.2m) and nursing (£4.1m). But in fact, we found, nearly a fifth of trusts spent even more than 10% of their total staffing bill on agency.
We found that 30 trusts out of 176 respondents (with the exception of three who refused to divulge their total staff bill because it was exempt under section 22 of the FoI Act), or 17.3%, had spent more than a tenth of their staff budget on agency.
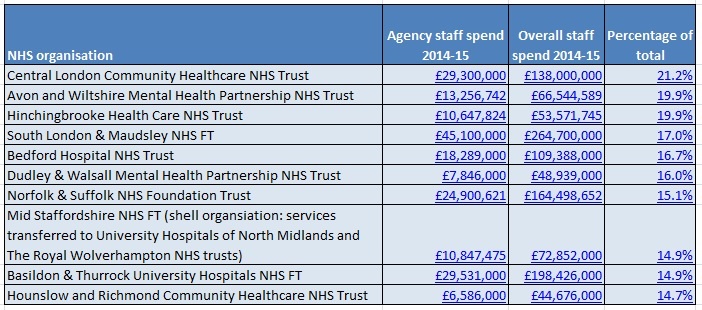
Central London Community Healthcare NHS Trust, which provides community and in-patient services to almost a million people in Barnet, Hammersmith & Fulham, Kensington & Chelsea and Westminster, spent £29.3m on agency staff (though did not break this down by staff type).
This represented 21.2% of the trust’s £138m total staffing bill. Cyndee Massa, information governance facilitator at the trust, told us it “did not budget for temporary staff costs” in 2014-15.
However, Avon & Wiltshire Mental Health Partnership NHS Trust, which spent 19.9% of its total staffing bill on agency supply, did provide a breakdown. The mental health trust spent £13.25m of its £66.54m staffing bill on agency, with the two largest spend areas being dominated, once again, by medical and nursing.
During the 2014-15 financial year, the trust had planned to spend £698,179 on agency nurses – it spent £9.8m. It overspent similarly on medical staff, managing to spend £2.2m when it thought it would need to spend £338,139.
In January, Circle Health decided to pull out of its contract managing Hinchingbrooke Health Care NHS Trust – the first privately run NHS hospital.
The trust was handed back to public hands in April, marking an unhappy end to the Department of Health’s biggest experiment in healthcare privatisation. And Hinchingbrooke currently remains rated overall as ‘requires improvement’ by the Care Quality Commission (CQC), with it receiving an ‘inadequate’ mark for being ‘well-led’.
In terms of its contract and agency staff spend, the trust spent just over £10.6m in 2014-15, more than double the planned £5.2m. The figure also represented 19.9% of Hinchingbrooke’s total staff expenditure.
 Candace Imison (pictured), director of healthcare systems at the Nuffield Trust, told NHE that the situation across the NHS is worrying. “The escalating spend on agency is of deep concern for two reasons. Firstly it inflates staff costs at a time when trusts are under huge pressure to contain them. Secondly a high dependency on agency staff is a threat to high-quality care and strong staff engagement.
Candace Imison (pictured), director of healthcare systems at the Nuffield Trust, told NHE that the situation across the NHS is worrying. “The escalating spend on agency is of deep concern for two reasons. Firstly it inflates staff costs at a time when trusts are under huge pressure to contain them. Secondly a high dependency on agency staff is a threat to high-quality care and strong staff engagement.
“While the government’s recent attempts to limit the rates charged for agency staff are to be welcomed, this does little to tackle the underlying causes. Action is needed to grow the supply of nurses but also to make the roles in ‘hard to recruit’ areas, such as care of the elderly, more attractive."
Clampdown
Since Monitor and NHS TDA revealed the overall agency spend figures, the health secretary has unveiled a package of tough new financial controls to clamp down on agencies, including plans to set a maximum hourly rate for agency doctors and nurses, banning the use of agencies that are not on approved frameworks, and requiring specific approval for any expensive consultancy contracts over £50,000.
Monitor has also set up a team of experts to run an initial three-month trial at three FTs to reduce the amount being spent on agency staff.
While NHE carried out our investigation into agency pay, the King’s Fund released its 16th quarterly monitoring report, which found that more than 60% of NHS trust finance directors think the controls on agency spending announced by Jeremy Hunt will “not significantly reduce” the amount spent on agency staff.
It found that three-quarters of trusts intend to recruit more permanent nurses in the next six months, suggesting that the NHS is continuing to prioritise quality of patient care despite rising financial pressures.
Talking to us about our results, Dr Rachael Addicott, senior research fellow at the King’s Fund, said: “In a sense it is really not that surprising, we can see that this is the direction of travel. We only looked at acute and mental health trusts, whereas you have data on community trusts, which is really interesting – but also not surprising, as we know overall that the community workforce is suffering the same (if not more) from the crisis around nursing staff as the acute trusts.
“Looking at this across acute, mental and community trusts, this is quite a wide-scale problem. I think the Department of Health measures are only tackling one problem: the cost of agency staff. But those measures aren’t really tackling the problems around the supply of nurses that we can see now. This has historically been a problem in the acute sector. We saw that it was starting to be a problem in mental health as well and you have information on community nursing, showing that there aren’t enough nurses out there. Putting curbs on the cost of agency staff is really only tackling one angle of the problem, and is not likely to lead to any large-scale change in the workforce.”

On hearing of our findings, Danny Mortimer, chief executive of NHS Employers, told us that there is some potential for NHS trusts to cut spend on agency workers through further improvements in flexible working, technology and arrangements with local agencies.
“NHS trusts also need to recruit permanent staff from other countries,” he said. “This is a responsible approach to recruitment and reducing agency spend and needs continued support from across the government. Patient safety is our absolute priority and it’s important to remember that agency staff are useful for ensuring continuity and quality of care. In controlled, smaller numbers agency and bank staff will have a long-term future helping the NHS respond to fluctuations in demand.”
A system ‘under significant pressure’
Rob Webster (pictured), chief executive of the NHS Confederation, added that we are seeing a system “under significant pressure” which is demonstrated most intensively in acute trusts, with widespread performance challenges and almost nine out of ten predicting a deficit this year. _PAGE_28_Option_1_edit.jpg)
“Short-term initiatives around agency staff and capping pay will make a contribution to NHS finances but will not be the whole answer,” he said. “But the NHS will need to explore all aspects of spending to tackle the big challenge of delivering £22bn of recurrent savings by 2020. We are working with national bodies and other NHS partners over the summer to bring our members closer into the discussion and to understand how the NHS might close the finance gap set out in NHS England’s Five Year Forward View.”
In June, Lord Carter’s ‘Review of Operational Productivity in NHS providers’ revealed that in 2013-14, the cost of nurses in the NHS was £19bn. But with the increased focus on safer staffing and a 29% increase in the rate of nurses leaving the profession in the last two years, the dependency on agency nurses has risen significantly – doubling between 2012 and 2014.
His report mentioned the health secretary’s proposals, but added: “We need to place more focus on the root causes of the increased demand for such services.”
Speaking to NHE in an interview at the Treasury, Lord Carter suggested that running a good work bank and looking at the rates being paid are critical factors in making sure trusts are not overly reliant on agency staff.
He added that since Mid Staffs, some trusts have been practising ‘defensive nursing’ in quantity terms.
“So, some people are taking agency when they don’t need it,” he said. “We’ve data to show that. One hospital in our cohort re-did all its policies around rotas and moved from a shortage of nurses to having 27 too many. There is an argument that says if you use our resources really well you shouldn’t need institutionalised agency. Plus, one of our hospitals let everybody go off on half-term; they didn’t have a roster policy saying you can’t go.”
Under-spenders: how did they do it?
Of all the respondents who budgeted for agency spend, only three trusts underspent on their forecasts: Manchester Mental Health & Social Care Trust; Cornwall Partnership NHS FT; and South Essex Partnership University NHS FT.
According to the FoI return, Manchester expected to spend £8.6m out of its £76.5m staffing budget on agency staff. But it actually only spent £7.75m– so £859,811 lower than forecast (but still 10.1% of its overall staffing expenditure).
NHE asked the trust how it had managed to deliver this, but unfortunately a spokesperson only said: “Expenditure on agency was less than we initially thought it could have been at planning stage. As always, the trust is working hard to reduce agency expenditure, though it can be noted that we do not see that it was an under-spending against budget.”
There were, however, concerted efforts made to reduce reliance on agency staffing in Cornwall, which has become the first county to benefit from a devolution deal with the government. Cornwall Partnership NHS FT, the principal provider of mental health, children's and learning disability services to people in Cornwall and the Isles of Scilly, had originally forecast to spend £1.3m on agency staff.
But our FoI investigation revealed that it managed to spend £425,000 less than expected, with agency expenditure coming in at just over £909,000. This represented only 1.52% of the FT’s £60m staffing budget.
Sharon Linter, executive nurse at Cornwall Partnership NHS FT, told us: “Our success in managing our use of agency staff and the amount we spend in this area is attributable to our renewed focus on recruitment and roles.
“To achieve this, we reviewed job descriptions, looked at the way roles are structured and targeted our recruitment campaigns accordingly. For example, we have increased the numbers of preceptor roles for newly qualified nurses, to attract fresh talent into the trust. This not only brings new ideas but allows newly qualified staff to benefit from the experience of long-serving staff. We have also introduced apprenticeship roles across the organisation.
“We have further developed our own staff ‘bank’, recruiting people who want to work flexibly within their local community. This ensures we have a group of trained staff who are familiar with our wards and facilities who cover shifts at short-notice. Our board also regularly monitors our staff turnover and agency use.”
South Essex Partnership University NHS FT did not respond to our request for comment.
Banking on it
Discussing the use of bank staff versus agency staff, NHS Professionals, the NHS-owned organisation that manages temporary staff banks on behalf of more than 60 trusts across England, told us: “The gap between the number of people who need care and those available to deliver care continues to grow, creating a space in which expensive staffing agencies can thrive.”
Its chief executive, Stephen Dangerfield, said one way to cut agency spend is for the “NHS to work collectively to stamp out practices such as allowing staff to work through external staffing agencies rather than the trust’s own bank”.

But the Recruitment and Employment Confederation (REC), which supports and advises agencies across health and care, said agencies are not “ripping off” the NHS.
“The majority of NHS trusts manage their agency spend through framework agreements, which already cap prices. Rates are negotiated by central government and recruitment agencies must adhere to them,” said Kate Shoesmith, head of policy at the REC.
The King’s Fund’s Dr Rachel Addicott told us: “I am aware that Monitor and NHS Employers are working with trusts to try to help them think about how they can retain the staff they’ve got and recruit some more permanent staff as well.
“I think bank could really be a good opportunity to tackle this issue. However, it doesn’t solve the problem completely. But it does provide some kind of continuity: those staff on the bank already know the organisation, having worked regular bank shifts on the same ward etc. Therefore, all the implications that continuity of care has around patient safety could be really important.
“There are initiatives out there to encourage more staff to take on bank shifts, but it is not particularly widespread at the moment.”
Siva Anandaciva, head of analysis at NHS Providers, told NHE: “The use of agency staff has a legitimate role in ensuring that our members can provide patients with the care they need. However, the regulatory and political climate has compelled NHS providers to make greater use of bank and agency staff at a considerable premium rate and this is simply not financially or clinically sustainable.
“We welcome any helpful guidance and support that shares best practice in managing agency spending, such as Monitor’s recent business plan for the Agency Intensive Support Team, but this must be coupled with national action to tackle the fundamental mismatch between supply and demand that has driven this reliance on agency spend in the first place.”
To access the full set of data and FoI responses, click here.