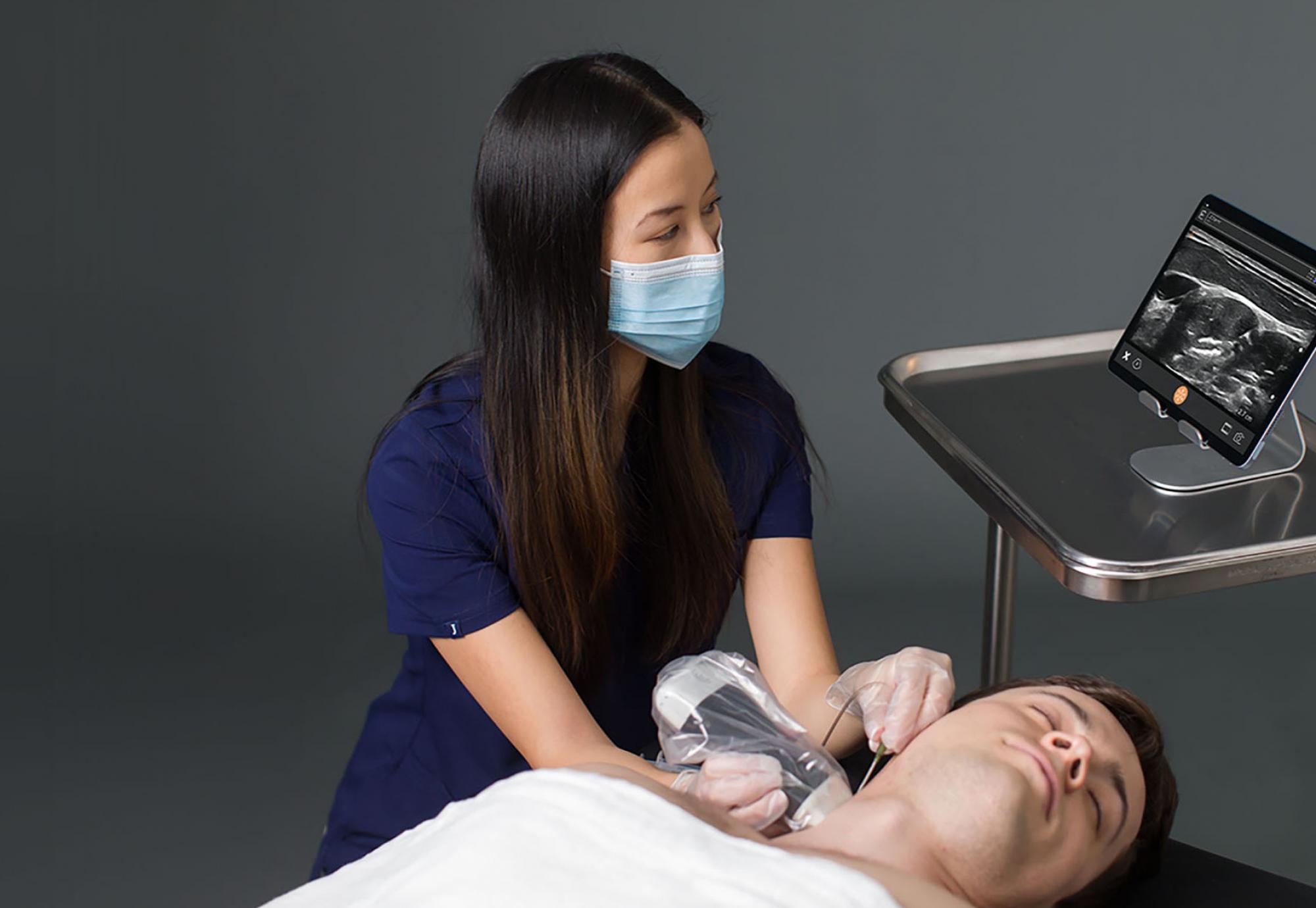
Practitioners are always looking for better tools to help them improve patient outcomes. In 2023, that tool will be ultrasound.
Medical imaging has long been used in hospital settings to evaluate patients and provide care. But ultrasound is on the move, and new high-definition handheld models have brought this technology out of radiology departments and into clinics, specialist offices, ambulances, and even patient homes.
But ultrasound has yet to reach its full potential. While many practitioners utilize the technology in their practice today, there are others who are hesitant to do so. In my over twenty years in the medical device industry, I've spoken to thousands of practitioners who see the benefits of ultrasound, and its potential will only be unlocked when practitioners view it as a tool more critical to patient care than a stethoscope.
What should practitioners know about ultrasound in 2023? Here are five insights into the current state of ultrasound usage based on practitioner input, and what you should know if you're considering bringing ultrasound into your practice.
Five Insights into Ultrasound
Ultrasound can be a transformative tool in the hands of a practitioner, and the global portable ultrasound market is expected to reach $3.8 billion by 2031. In order to better understand the state of ultrasound — adoption, sentiments, and usage — we surveyed 687 physicians in various specialties for our recent "State of Ultrasound 2023" report. They gave us the following insights about ultrasound today that can help you better understand the technology, the hurdles to adoption, and the benefits it can bring to patient care.
1. 85% of practitioners believe that ultrasound leads to better patient outcomes.
The vast majority of practitioners agree that using ultrasound in their practice improves patient outcomes. First, they see its benefit in diagnosing patients. By being able to see into a patient's body in real time, they can get answers to diagnosis questions immediately, instead of having to wait days or weeks for off-site imaging. Using ultrasound for assessment gives much more insight and information than a stethoscope, and as a recent piece in The New Yorker boldly asserted, “Stethoscopes were just for doctors. Ultrasound could be for everyone.”
Practitioners also see its benefits in treatment, making procedures more accurate and safer when they can clearly see anatomy beneath the skin. For example, fat grafting procedures done incorrectly can lead to injury and even death; now practitioners can are assuring a much safer procedure by using ultrasound to guide their way — so much so that the Florida Medical Association requires any fat grafting procedures to be done under ultrasound guidance.
2. 86% have an ultrasound machine at their practice.
If 85% see the benefits that ultrasound brings to patient care, then it makes sense that 86% of practitioners have an ultrasound machine in their office — either a large cart-based system, a compact or laptop-based system, or a handheld device. Additionally, 87% said they plan to purchase additional ultrasound machines in the next year, either to help offer more services to patients or to upgrade their legacy systems with newer, affordable, and more portable handheld devices.
3. Expanding services is the top driver for incorporating ultrasound into a practice.
Specialists with private practices constantly need to think about the services they provide, and the primary driver for incorporating ultrasound into their practice is to do just that. As specialists add services that can best help their patients — more aesthetic procedures, for example, or pain management offerings — they're adopting ultrasound as a way to make those services safer and more effective.
But ultrasound can also be used to differentiate a growing practice, as an increasing number of patients are searching for practitioners who use ultrasound to deliver procedures accurately and painlessly. A recent report found that patients who experience point-of-care ultrasound “felt that they had been more thoroughly examined and taken more seriously,” and ultrasound “improved the level of service they experienced and the quality of care in general practice.”
4. Not being trained in ultrasound is the primary reason for not having one.
Those who don’t have an ultrasound machine in their office say it’s because they're not trained to use it. But considering that nearly all said they have some kind of training in ultrasound, it's not simply a broad lack of training that's the hurdle. If they learned ultrasound during their internship or residency, or even as far back as med school, they may have lost the skill and see "brushing up" as too time-intensive. Or, they may have learned ultrasound in one specialty, yet practice in another where they haven't yet learned how to apply ultrasound.
Whatever the case, there may not be as steep a curve as some may think. Today there are many third-party websites and organizations offering ultrasound training, and some practitioners I've spoken to are even self-taught from YouTube videos. Today's handheld devices also contain AI guidance, which trains a practitioner as they're using it. And simply using ultrasound can increase proficiency, as “ultrasound helps students learn the location and relationships between anatomical structures and their disposition in a living human body, strengthening their cognition and concepts of anatomy.”
5. 89% believe that all clinicians should be trained in ultrasound.
Finally, most practitioners surveyed believe that all clinicians should be trained in ultrasound. Not only did emergency physicians and cardiologists — power users of ultrasound — believe their colleagues should be trained in ultrasound. Respondents including plastic surgeons, orthopedic surgeons, and cosmetic dermatologists also believed that those in their specialty should be trained as well. These are specialties that traditionally never used ultrasound — however, as more practitioners understand its benefits, we're seeing a shift in prioritizing ultrasound training and usage in these specialties.
Engaging with Ultrasound Today
These key insights point to one thing: ultrasound can play a key role in improving patient outcomes, and newer, high-definition handheld devices are allowing practitioners to use ultrasound in many different settings and specialties. Practitioners are always looking for better tools to help them improve patient outcomes, and it’s clear that tool is ultrasound.
Author’s bio:
Ohad Arazi is the President and CEO of Clarius, a leading provider of high-definition wireless ultrasound systems. Ohad has over 20 years of experience in the digital health, medical device, and telecommunications industries as an entrepreneur, public company executive, and CEO. Prior to Clarius, Ohad served as CEO of Zebra Medical Vision, an Israeli imaging AI company backed by Khosla Ventures, Intermountain, Marc Benioff, and strategic investors such as TELUS Ventures. Prior to joining Zebra Med, he was the CSO for TELUS Health, where he oversaw the Provider Solutions Business Unit. He oversaw the organization's expansion to provide Electronic Medical Record systems to 28,000 primary care physicians across Canada, as well as the launch of Canada's first electronic prescribing network. Before joining TELUS in 2017, Ohad was Senior Vice President and General Manager for Change Healthcare and McKesson's cardiology business, both of which are among the top three global market leaders in medical imaging software.