Accessibility is something we see all around us from lowered door handles to ramp access and disabled changing rooms with additional space for wheelchair users.
Hospitals and clinical settings are where we would perhaps think to find most of these accessible features, supporting not only patients but staff as well.
While we evolve our current NHS estates into more efficient, environmentally friendly spaces and build new buildings to incorporate technology and digital innovations, is accessibility at the forefront of our minds and should we spend more time understanding some of the issues that people with accessibility needs can face on a daily basis?
Grace Spence Green and Ras Kahai are both based in clinical roles at Guy’s and St Thomas’ NHS Foundation Trust. Grace is a newly qualified junior doctor at St Thomas’ Hospital and Ras is a cardiorespiratory dietitian at the Royal Brompton Hospital & Harefield hospitals and are both wheelchair users.
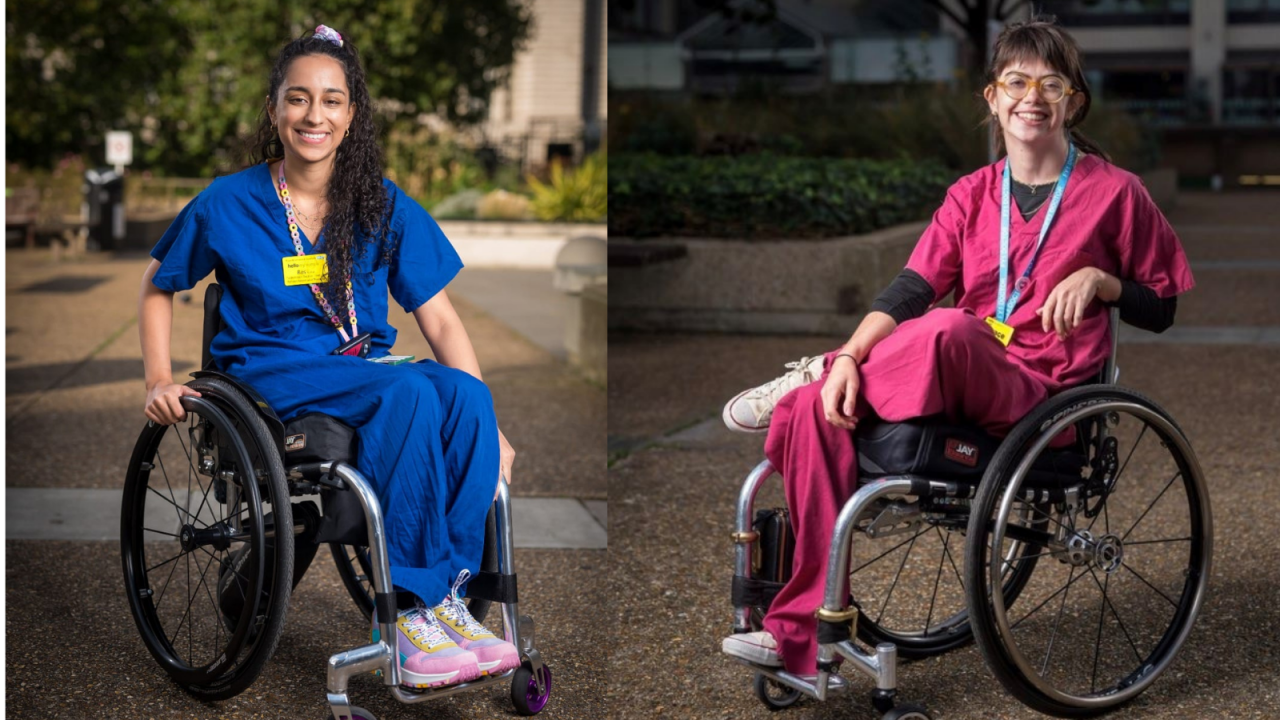
For both Grace and Ras their day-to-day work routine is the same as their other colleagues, but Grace thinks that one of the main issues that she faces daily is the stigma around disability.
“I find that people constantly underestimate my abilities. I’m not recognised for the role I play in the hospital. I’m always being mistaken for a patient and it’s really strange to me because I’m wearing scrubs and a stethoscope and lanyard, but that’s not enough. They see the wheels and that’s it.”
The Equality Act 2010, previously known as the Disability Discrimination Act (DDA), ensures that organisations make reasonable adjustments to allow access to goods, facilities and services. Included within this act is the requirement to make all doors accessible anywhere where a disabled person may require access.
In addition to her clinical role, Ras also co-chairs Royal Brompton and Harefield’s Disability and Wellness Network (DAWN), which promotes equality and inclusivity for disabled staff, and works with departments across the hospitals to improve physical access for disabled patients, visitors and staff.
Ras explained that while most doors have handles at the correct DDA height, mask holders and scrub racks were often not. She said: “I think there needs to be some sort of link, between lived experience of disabled patients & staff with the estates team who work on accessibility.. Mask holders were put up too high and not at an accessible height. I had to advocate recently to get them moved down, which estates managed to change, but it’s about having that anticipatory thinking and I think the entire workforce could be upskilled on that a little more.”
Pedal bins are another object in the hospital that Ras has found to be more challenging for her to use. The hospital is currently trialling 20 new bins in non-clinical areas which also have handles. “Putting PPE in bins was really hard for me during the pandemic,” said Ras. “While we are trialling these new bins it is only in non-clinical areas for now, so we still don’t have a solution for clinical areas yet”.
Ableism in the workplace has been highlighted recently as the government pledged to work towards increasing the number of disabled people in employment after releasing statistics for the previous year.
Grace said that a main concern of hers among stigma around disabilities was ableist language. “Unfortunately, I’ve found that [ableist language] comes from colleagues and other workers in the hospital rather than patients.
“For patients, I think because I have such a visible scar, and they understand I’ve probably spent time in hospital, they can relate to me and be more open.
“I find that colleagues sometimes get really uncomfortable. They worry about saying the wrong thing so much that they end up saying the worst possible thing. I’m quite confident in correcting people and saying please don’t use ‘wheelchair bound’ or saying ‘I don’t have special needs’, say I have access needs instead.”
“I think it’s indicative of a bigger issue we have in society. People can’t seem to wrap their heads around that while I am a disabled person, I am also a person in a position of power and a position to care for others”.
In the NHS Workforce Disability Equality Standard (WDES) annual report 2019, data revealed that only 2.9% of clinical staff were disabled.
Grace added that after her spinal injury in her fourth year of medical school she didn’t feel like she could return to her studies as a doctor until she met another doctor who was a wheelchair user.
Like Ras, Grace has also taken on another role in her spare time outside of the hospital by teaching current medical students about disabilities and helping them to understand how best to care for and speak to disabled patients. “It’s not only that, but also working with disabled colleagues”, said Grace. “I think that it’s really important and those are skills that I really appreciate.”
In her role as co-chair for DAWN, Ras has been advocating better accessibility for both staff and patients around the hospitals.
“We brought some of the directors to the hospital to come around with me in a wheelchair, not for disability simulation but to look at mobility around the site and how the hospital environment can be disabling towards mobility aid.
“We now have a protected, ringfenced budget to spend on accessibility projects such as changing places, toilets and additional chairs around the hospitals for people to sit on if they get tired or fatigued,” said Ras.
Access guides for Guy’s Hospital and St Thomas’ Hospital are already available online. The specialist website takes photographs of various areas around the site and then creates an accessible guide for patients and staff to follow when visiting. It allows visitors to see doorway widths, floor types and much more before arrival to make it an easier experience to navigate.
Access guides for Royal Brompton and Harefield hospitals have launched this week.



















