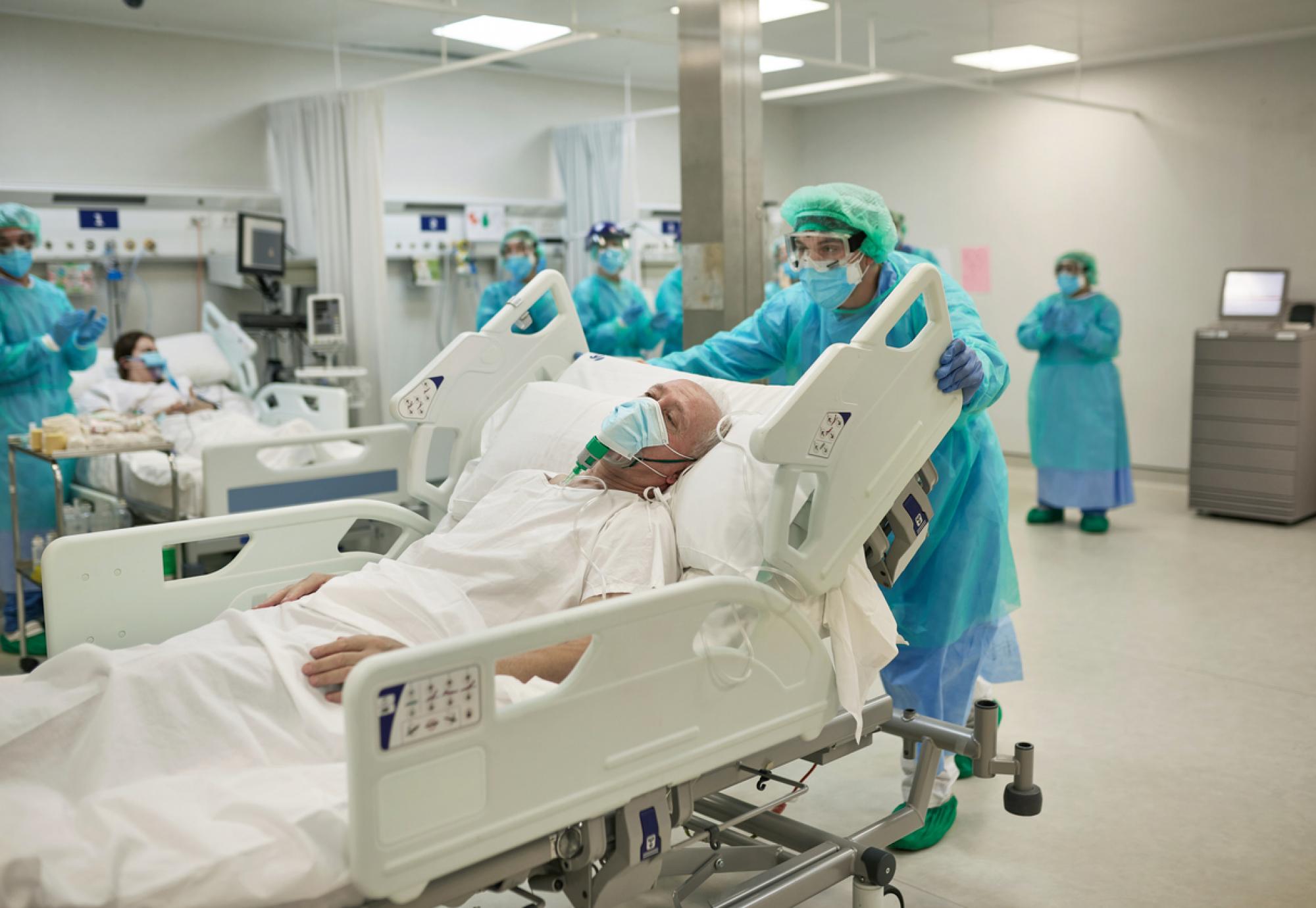
Ensuring that hospitals are equipped with the best protection, and the right measures are in place when it comes to infection prevention and control, have become essential during the pandemic. This has been especially apparent when protecting vulnerable groups.
Dr David Nicholl, Consultant Neurologist at Sandwell and West Birmingham Hospitals NHS Trust, spoke to NHE about the main discussion points ahead of the NHE365 event on 23 June. He will present the opening keynote speech on the lessons learned from his experience as a neurologist on a stroke/neurology ward.
The main areas Dr Nicholl will talk about are:
- The study he was involved in: Nosocomial spread of Covid-19: lessons learned from an audit on a stroke/neurology ward in a UK district general hospital.
- Looking at Asia as an example for improving IPC practices.
- The link between increased community rates and HAIs.
- The challenges regarding vulnerable patients at a higher risk, such as those with brain injuries.
He discussed the outbreak of nosocomial Covid on his trust’s ward, issues that were present at the time, and what that means moving forward. This also included looking at Asia as an example of what the sector should aspire to when it comes to ventilation.
Dr Nicholl explained: “We had an outbreak of nosocomial Covid on our ward in the first wave of Covid, and this was at a time when testing availability was quite limited.
“But it had an absolutely colossal impact on us as a service, and then something like 19 members of staff ended up with Covid or became very ill. Fortunately, no one died, but it made us think a lot about nosocomial Covid and the lessons we learned from that.
“Now, obviously it’s much easier with testing and vaccines. But I think the most important thing is not being complacent, and in many ways just looking at what other countries have done well, such as Asia and South Korea being really obsessive about everything.”
He highlighted how having more awareness surrounding the link between HAIs and the increased rates in communities, would help better protect patients, and what was learned regarding the process in hospitals.
He commented: “When Covid rates go up in the community, it is almost inevitable there will be higher rates within the hospital as well, and you just need to keep reminding people to follow the processes really.
“There’s been a lot of debate about individual items such as PPE, social distancing, and everything else. But actually, it’s doing all of it and continuing to do it, so it’s not only one thing, which is why we kind of made the analogy of trying to get Sandwell like South Korea.”
He shared the need for more transparency when sharing HAI data, and how better understanding of this could lead to improved responses when dealing with an outbreak.
Dr Nicholl commented: “When you get more Covid in hospital, you can be doing absolutely everything perfectly, but there will still be a risk of Hospital acquired Covid. So, I think that data should be in the public domain and in trust board papers, in the same way as we would for MRSA or c. difficile.”
Dr Nicholl also spoke of some of the reasoning behind the study, and the vulnerability of those with brain injuries who were more at risk of Covid, as well as the need to communicate well with staff to be able to manage outbreaks in the best possible way.
He concluded: “When we saw the outbreak, I felt it was very important actually to engage with the junior staff dealing with an ineffective call to improvement project. So, I thought, well let’s track where our patients have been and see how this outbreak had spread, and what we can learn from it.
“So, I think we basically need to act like South Korea did in 2020 by thinking about ventilation, and I think that is a massive challenge as we look ahead actually in terms of hospital designs, and there’s no easy answer.”
Join Dr Nicholl and many other healthcare professionals at NHE365’s Infection Prevention & Decontamination event on 23 June. You can register for the event here.