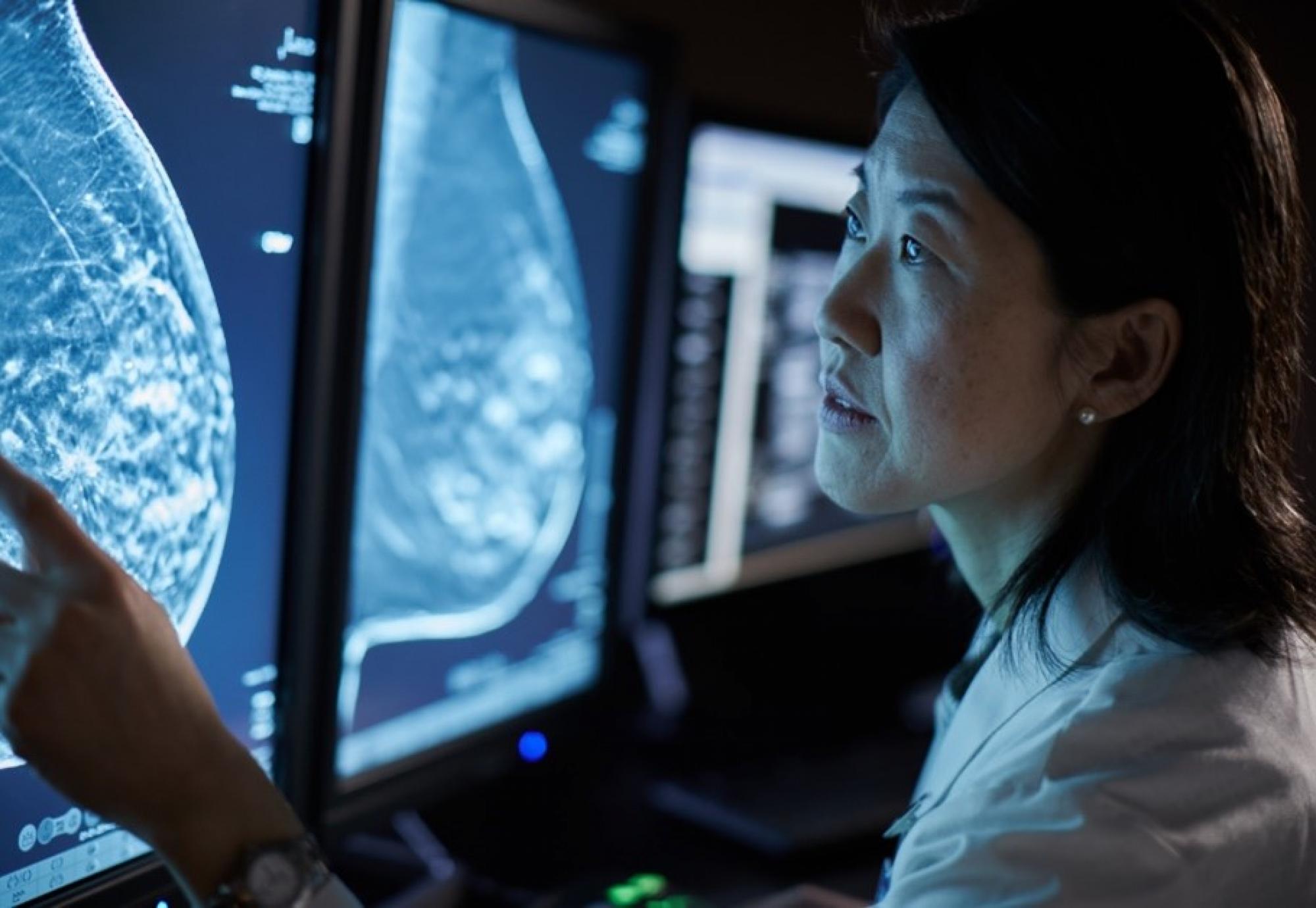
What is the biggest challenge to the national breast cancer screening programme?
The biggest challenge is the shortages of radiologists. According to the 2020 annual census from the Royal College of Radiologists (RCR), in the UK there is a staff shortage of approximately 33%, so nearly 2,000 more radiologists are needed to ensure appropriate services are provided[1].
Furthermore, unless further steps are taken, the RCR forecasts the shortfall will hit 3,600 by 2025 (equivalent to 44% of the current workforce) as 26% of radiologists will retire1.
How can technology improve the mammography service workflow?
Tools such as the Hologic Genius AI™ Detection* deep learning technology may assist radiologists in the detection of breast cancer by identifying suspicious lesions that could potentially be cancerous. AI solutions such as this could enable operational efficiencies, providing the breast screening service with greater productivity using the workforce it already has.
Other new technologies such as 3DQuorum™ have the potential to improve mammography workflows, particularly alleviating pressures on image interpretation and reporting, by reducing the Picture Archiving and Communication System (PACS) storage requirements for tomosynthesis images as well as helping radiologists prioritise patients, seek second opinions in real time, and turn around diagnoses for patients more quickly.
Digital breast tomosynthesis (DBT) together with other forms of smart technology, could not only transform breast screening services but also play an important role in workflow prioritisation, which could bring greater certainty to patients and clinicians, as well as helping address staff shortages. DBT and the use of AI also have the potential to increase breast cancer screening capacity, by removing the need for review by two radiologists.
What impact could this smart technology have on patients?
New AI technologies could assist with the speed and accuracy of reporting, ensuring patients get answers as quickly as possible.
While false positives lead to unnecessary recalls and further anxiety for the patient, an even more disturbing aspect is that 15 to 30% of breast cancers are not detected by standard 2D mammography[2], which is why it is important for the implementation of digital breast tomosynthesis (DBT) to be considered within the screening programme. Studies have shown that DBT, when compared to traditional 2D mammography, detects up to 65% more invasive breast cancers, and reduces patient recall by up to 40%[3],[4].
These smart technologies can also play a large role in risk stratification for women with dense breast tissue who are known to be at particularly high risk of developing breast cancer.
AI machine learning and deep learning technologies could be used to analyse the prior mammograms of women retrospectively and identify those at greatest risk. Almost 43% of women over 40 years old have dense breast tissue that can obscure lesions on traditional 2D mammograms, making cancers harder to detect and recalls more likely[5]. Women with very dense breasts have a four to five times greater risk of developing breast cancer in comparison to women with less dense breasts[6] .
New AI–powered technologies have the potential to help identify and prioritise women who are particularly at high risk of breast cancer, creating a more efficient and personalised breast screening programme in the longer term.
*Not CE Marked. Not available for sale yet. Not for distribution.
Disclaimer
Views and opinions expressed herein by third parties are theirs alone and do not necessarily reflect those of Hologic.
Hologic, Inc. All rights reserved. Hologic, The Science of Sure, and associated logos are trademarks and/or registered trademarks of Hologic, Inc. and/or its subsidiaries in the United States and/or other countries. All other trademarks, registered trademarks and product names are the property of their respective owners.
[1] The Royal College of Radiologists. Clinical radiology UK census 2020 report. London: The Royal College of Radiologists, 2021. Available from: https://www.rcr.ac.uk/publication/clinical-radiology-uk-workforce-census-2020-report
[2] Gilbert FJ, Tucker L, GC Gilian M. Accuracy of Digital Breast Tomosynthesis for Depicting Breast cancer subgroups in a UK retrospective reading study. Radiology: Volume 277: Number 3, 2015
[3] Friedewald SM, Rafferty EA, Rose SL, Durand MA, Plecha DM, Greenberg JS, et al. Breast cancer screening using tomosynthesis in combination with digital mammography. JAMA. 2014 Jun 25;311(24):2499-507.
[4] DiPrete O, Lourenco AP , Baird GL, Mainiero MB. Nov 2017. Mainiero. Screening Digital Mammography Recall Rate: Does It Change with Digital Breast Tomosynthesis Experience?. Radiology: Volume 286: Number 3—March 2018
[5] Sprague BL, Gangnon RE, Burt V, et al. Prevalence of mammographically dense breasts in the United States. J Natl Cancer Inst. 106(10), 2014.
[6] Schreer I. Dense Breast Tissue as an Important Risk Factor for Breast Cancer and Implications for Early Detection. Breast Care (Basel). 2009 May; 4(2): 89–92.