30.11.15
Improving outcomes with data
Source: NHE Nov/Dec 15
 Ian Davison, business information services director at the North of England Commissioning Support Unit, discusses how using data can improve outcomes.
Ian Davison, business information services director at the North of England Commissioning Support Unit, discusses how using data can improve outcomes.
At the NICE Annual Conference in Liverpool in October, delegates were told about how sharing sensitive data and using medicine dashboards can improve outcomes for commissioners, care providers and patients.
In particular, North of England Commissioning Support Unit’s (NECS’s) business information services director Ian Davison outlined the organisation’s business intelligence tool: RAIDR (Reporting Analysis & Intelligence Delivering Results).
Launched six years ago to support practice-based commissioning, RAIDR gives local clinicians self-service access to “robust, wide-ranging and up to date patient level information”.
It has been adopted by 45 CCGs, 1,700 GP practices, one foundation trust, and covers a population of approximately 11 million. Davison told NHE: “We started it over six years ago, and it is not finished and never will be finished because we constantly improve it.”
Discussing RAIDR’s future, he told us that NECS intends it to be a single version across a health economy. “Accountable care organisations are the next big thing,” said Davison. “So we are building a version of RAIDR which expands from where it is at the moment, with the main focus being on commissioning and primary care, into secondary care, community and mental health etc.”
The tool, developed out of the need for GP practices to utilise the wealth of available NHS data, has also been approved by the Government Procurement Service under the new G-Cloud VI framework.
“We’d love to be providing it to a broader audience. It has expanded…it is now [covering] 20% of the country,” he said. “But we would like it to be more and we think we have the best tool out there.”
Learning to share
Its development is informed by its customers and user group, chaired by one of its CCG users. Asked what the difficulties have been in developing the tool, Davison said the biggest problem has been data – sharing and accessing it. Despite having access to a range of data sources, NECS has had to build relationships over the years with trusts “so they provide data directly to us, rather than going through the SUS (Secondary Uses Service) engine”.
This includes emergency admissions, A&E data and discharge data, which is then made available to commissioners and GP practices. Davison said this has only been possible by explaining the entire benefits to everyone in the health economy, which takes time.
He also noted that “crucially” NECS has built RAIDR’s reputation by being strict with what it does with the data and who can access it.
“We have had lots of people, over the years, requesting data because they are in certain positions,” said Davison. “But because of the T&Cs of the agreement they are in we haven’t gone beyond or outside them. That builds up trust, but takes time to deliver.”
RAIDR now provides a system-wide view of urgent care activity, to improve patient management by presenting it in flexible, fast dashboards, noted Davison.
The current dashboards include:
- Secondary Care (inpatient, outpatient, A&E and 111 data)
- Urgent Care
- Primary Care
- Finance & Contracting
- Quality and Performance
- Prescribing
- Summary Activity
- QoF
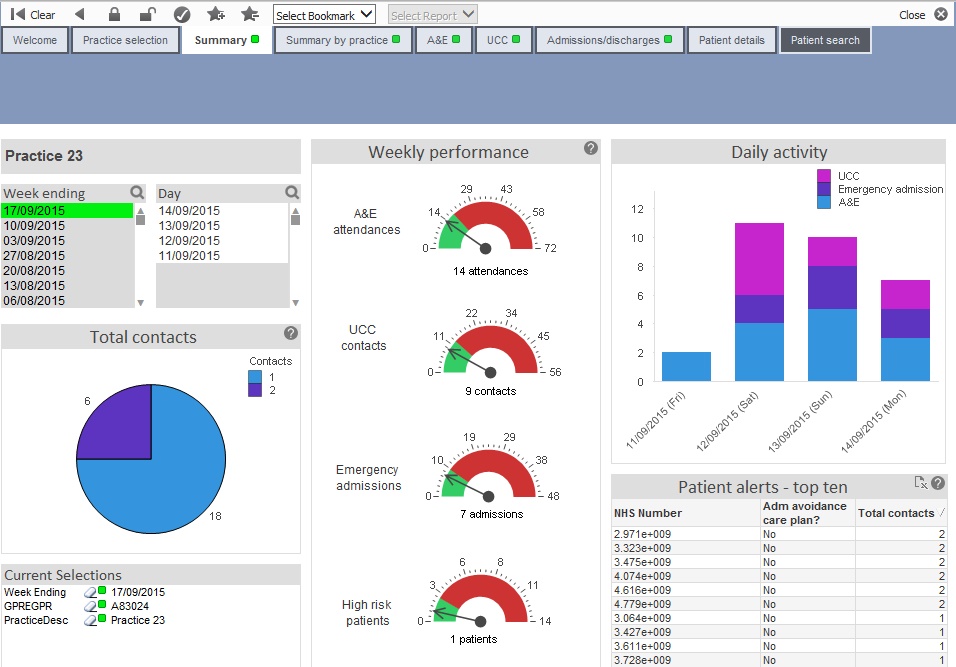
Davison also highlighted how the analysis tool is helping in practical terms. For instance, a GP user in the north east was able to quickly identify anomalies between hospital and practice diagnosis in dementia.
“So patients diagnosed in secondary care are now on the practice register,” said Davison. “Obviously, dementia patients are potentially vulnerable in the community, but he has now found dementia patients, which he didn’t know about, and can help to treat them.”
Saving lives
The same practice also noted that lives could be saved through the identification of untreated AF (atrial fibrillation). “Within a few clicks, the GP identified nine patients with potential AF who weren’t being treated within the practice,” noted Davison. “If he had clicked once more this would have been filtered down to four, which is what happened when he emailed practice people. They came back and said five people could be discounted because they had declined treatment or stopped smoking. The remaining four are then four potential lives saved.”
There is a team of 19 continually improving and supporting the system, which has been expanding with the customer base, noted Davison.
Asked what has made RAIDR popular, he said the roadmap and developments have been informed by user feedback. “We’ve also made the most of the business intelligence tool, with an effective development process, using the right technology and security so people can access what they need, while still being flexible and secure.”
Tell us what you think – have your say below or email [email protected]