29.11.17
Ten lessons to support new care models locally
Anna Starling, policy fellow at the Health Foundation, offers the top 10 lessons for local leaders seeking to make systematic improvements across services, all based on first-hand accounts from vanguard officials.
Redesigning health and social care services across traditional boundaries is not easy. Making change in complex environments, with differing professional viewpoints and varying organisational priorities while getting on with the job of delivering safe, effective health care is a huge task. And yet, in these challenging circumstances health and social care staff are redesigning services, determined to improve care for people whose care may otherwise have fallen through the gaps created by service fragmentation.
The New Care Models programme’s vanguard sites are examples of areas that are doing the demanding work of attempting to improve services across organisations. Supported with modest funding and access to expert advice from a national programme team led by NHS England, they have built on years of work prior to being designated as vanguard sites to redesign care for their local populations. This has predominately been for older people, those with chronic conditions and those with higher risk of admission. The sites did this by creating new teams and roles, new ways of sharing information and new locations for providing treatment.
The programme, however, ends in March 2018 and already appears at risk of becoming old news. The national spotlight is now firmly fixed on the creation of sustainability and transformation partnerships (STPs) and accountable care systems (ACSs). Yet those seeking to drive the development of new models of care within STPs and ACSs, at all levels of the NHS, can benefit from valuable learning from the vanguard sites.
In our new report, ‘Some assembly required: implementing new models of care,’ we set out 10 lessons for local leaders seeking to systematically make improvements across services in their area for those patients most in need of joined-up care. These lessons are based on first-hand accounts of clinicians and managers from the vanguard sites. Their approach to change emphasises the benefit of local co-creation and testing of new cross-organisational pathways and services before contractual solutions.
The lessons are underpinned by a strong focus on evaluation to understand what works and why. Not only to support the efforts of those implementing the changes, but also so that this learning can be shared across the health and social care system.
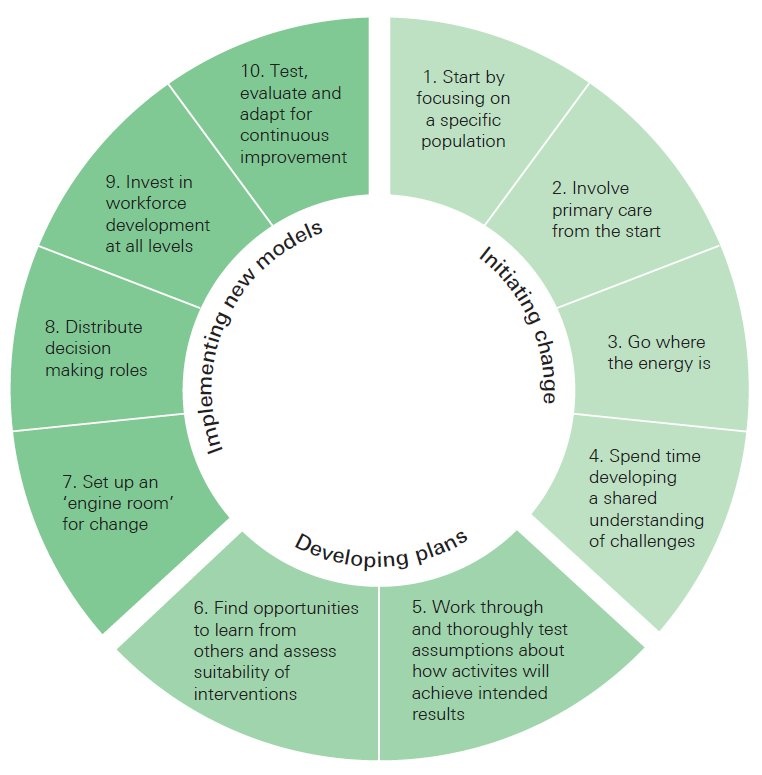
- Start by focusing on a specific population: Focusing first on a specific cohort of the population gives teams experience of co-designing services with patients and using data to understand need;
- Involve primary care from the start: Primary care plays an essential role in delivering coordinated care for patients, families and communities. General practitioners can offer significant insight into the needs of populations and where services can be developed;
- Go where the energy is: Identifying individuals and teams who already have ideas for and commitment to change can help gain momentum locally;
- Spend time developing a shared understanding of problems: Ensuring there is a shared understanding of the problems to be solved is a crucial factor in cross-team improvement work and requires that people are brought together at the beginning of any change initiative;
- Work through and thoroughly test assumptions about how activities will achieve intended results: Developing logic models can help teams think through and articulate links between planned activities and outputs without rushing to implementation;
- Find opportunities to learn from others and assess suitability of interventions: When looking at learning from elsewhere bring staff together to work through how to adapt the interventions for the local area;
- Set up an ‘engine room’ for change: In the absence of formal organisational structures, it is important to put in place a central project team that includes project management, data analysis, communication and administrative expertise. This should include staff who have already worked in the local area to create confidence among stakeholders;
- Distribute decision making roles: Ensure decision making roles are allocated across organisations and professional groups – not just at the most senior level;
- Invest in workforce development at all levels: With the creation of new cross-organisational services, investment in developing people is crucial. This is necessary at all levels of the local system and requires a focus on individual skills, team development and training for those in leadership roles;
- Test, evaluate and adapt for continuous improvement: Giving teams licence to experiment is crucial to understand the impact of changes and to help shape plans as they progress. It’s important to make sure people and teams involved are given feedback and supported to alter plans when changes do not go as intended.
The desire to change the delivery of care to better meet the needs of those who require support across health and social care services is not new. A 1972 NHS white paper acknowledged that ‘a single family, or an individual, may... need many types of health and social care and those needs should be met in a coordinated manner.’ The fact that there have been so many policies to deliver change reflects the difficulty of making change happen in complex health and social care systems.
Although the New Care Models programme is drawing to a close in 2018, wider application of its approach to change could have a substantial impact on the health and care of the population.