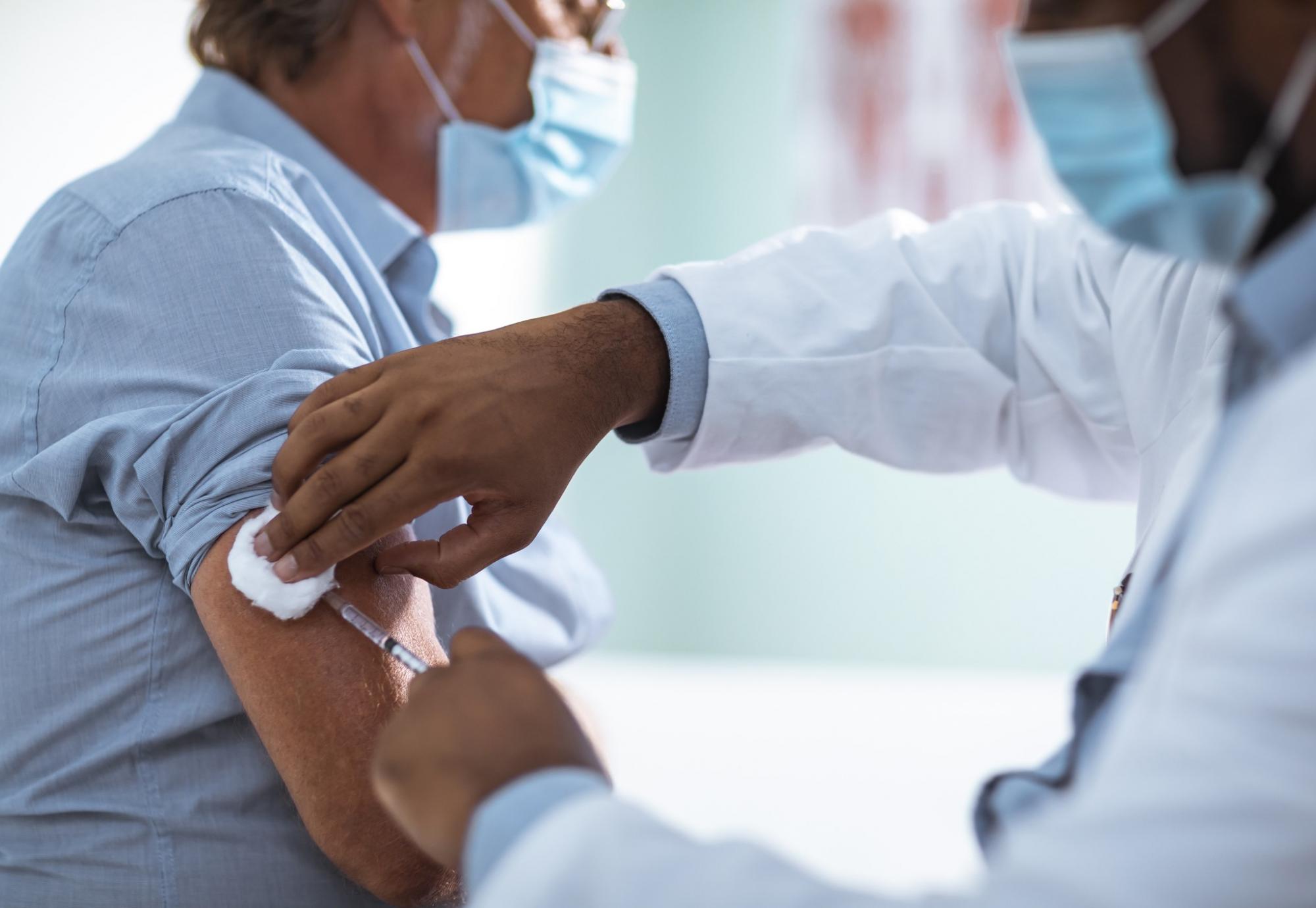
In order to better support the rollout of vaccines across the UK, a number of new laws have been introduced to allow more healthcare workers to administer flu and potential Covid-19 vaccines safely to the public.
The new measures aim to save thousands of lives through significantly increased access to vaccines against potentially killer diseases.
It will also support the Government’s plans for the roll-out of a potential Covid-19 vaccine, should one be proven to be safe and effective through robust clinical trials and approved for use by the regulator.
Following a public consultation, changes to the Human Medicines Regulations 2012 will come into force today, which will see us say:
- enable the expansion of the trained workforce who can administer Covid-19 and flu vaccines to improve access and protect the public. This will begin with those who already have experience in handling vaccinations but may currently work outside of NHS settings, such as independent nurses, allied healthcare professionals, paramedics, physiotherapists, pharmacists and student nurses and doctors. The expanded workforce will undergo a robust training programme to ensure patient safety is upheld to the highest standards
- implement reinforced safeguards to support the Medicines and Healthcare products Regulatory Agency (MHRA) to exceptionally grant temporary authorisation, pending the granting of a licence, for new vaccines and treatments needed to tackle public health threats - provided they meet the highest safety, quality and effectiveness standards and there’s a significant public health justification for doing so
Health Secretary Matt Hancock said: “The NHS has vast experience in vaccinating millions of people against diseases every year.
“These legal changes will help us in doing everything we can to make sure we are ready to roll out a safe and effective Covid-19 vaccine as soon as it has passed clinical trials and undergone rigorous checks by the regulator.”
Under NHS and local authority occupational health schemes, the number of fully-trained and experienced healthcare professionals capable of administering Covid-19 and flu vaccines will be increased, as well as efforts being made to further expand the workforce to administer these vaccinations to the public.
It will make it easier and quicker for patients and healthcare workers to access the vaccines they need, protecting them against potentially fatal diseases.
The Government plans have been specifically designed to ensure it does not detrimentally affect other services in hospitals and in GP and community services, drawing on a pool of experienced NHS professionals through the NHS Bring Back Scheme.
This has been designed to ensure timely access to other NHS services remains possible even as the vaccination programme efforts are stepped up.
Deputy Chief Medical Officer Professor Jonathan Van-Tam added: “Covid-19 vaccines are being developed at speed which, if successful, will save lives.
“All vaccines must undergo 3 stages of clinical trials and be assessed for safety and effectiveness by the regulator before they are given to patients.
“The measures outlined today aim to improve access and strengthen existing safeguards protecting patients.”
Should a vaccine for Covid-19 be developed prior to 2021, the new changes to the Human Medicines Regulations will bolster existing powers to enable the Medicines and Healthcare products Regulatory Agency (MHRA) to temporarily authorise supply for any treatment or vaccine needed to respond to a public health need.
It means that should any vaccine be found to meet the safety, quality and effectiveness standards set by the MHRA then vaccinations would be able to begin without needing to wait for authorisation from the European Medicines Agency, who – up until the end of the transition period in 2021, as part of the Brexit process – would have previously been the only body able to grant a license.
Read more about Brexit and it's impacts on healthcare through our dedicated Brexit Resource Hub: