The UK’s healthcare systems were “ill‑prepared”, “overwhelmed” and “came close to collapse” during the Covid‑19 pandemic, according to the third report from the UK Covid‑19 Inquiry, published today by Chair Baroness Heather Hallett.
The report – The impact of the Covid‑19 pandemic on healthcare systems of the United Kingdom (Module 3) – is the most detailed assessment to date of how Covid‑19 affected hospitals, primary care, community services and the people who rely on them. It concludes that while the NHS and care systems “ultimately coped, but only just”, the consequences for patients, families and healthcare workers were profound, long‑lasting and often catastrophic.
Module 3 examined the state of the UK’s healthcare systems across all four nations before and during the pandemic. The Inquiry found that the UK entered Covid‑19 with systems already understaffed, short of hospital beds and experiencing high bed occupancy. Alongside this, the system was already heavily reliant on overworked and exhausted staff and suffering from long‑standing capacity pressures.
This fragility had “profound consequences” once Covid‑19 cases began to surge. The Inquiry reports:
- Health systems were overwhelmed
- Many Covid patients did not receive the care they would otherwise have received
- Diagnosis and treatment for non‑Covid patients were delayed, with some conditions becoming inoperable
- Healthcare workers faced unacceptable risks, including working in insufficient PPE
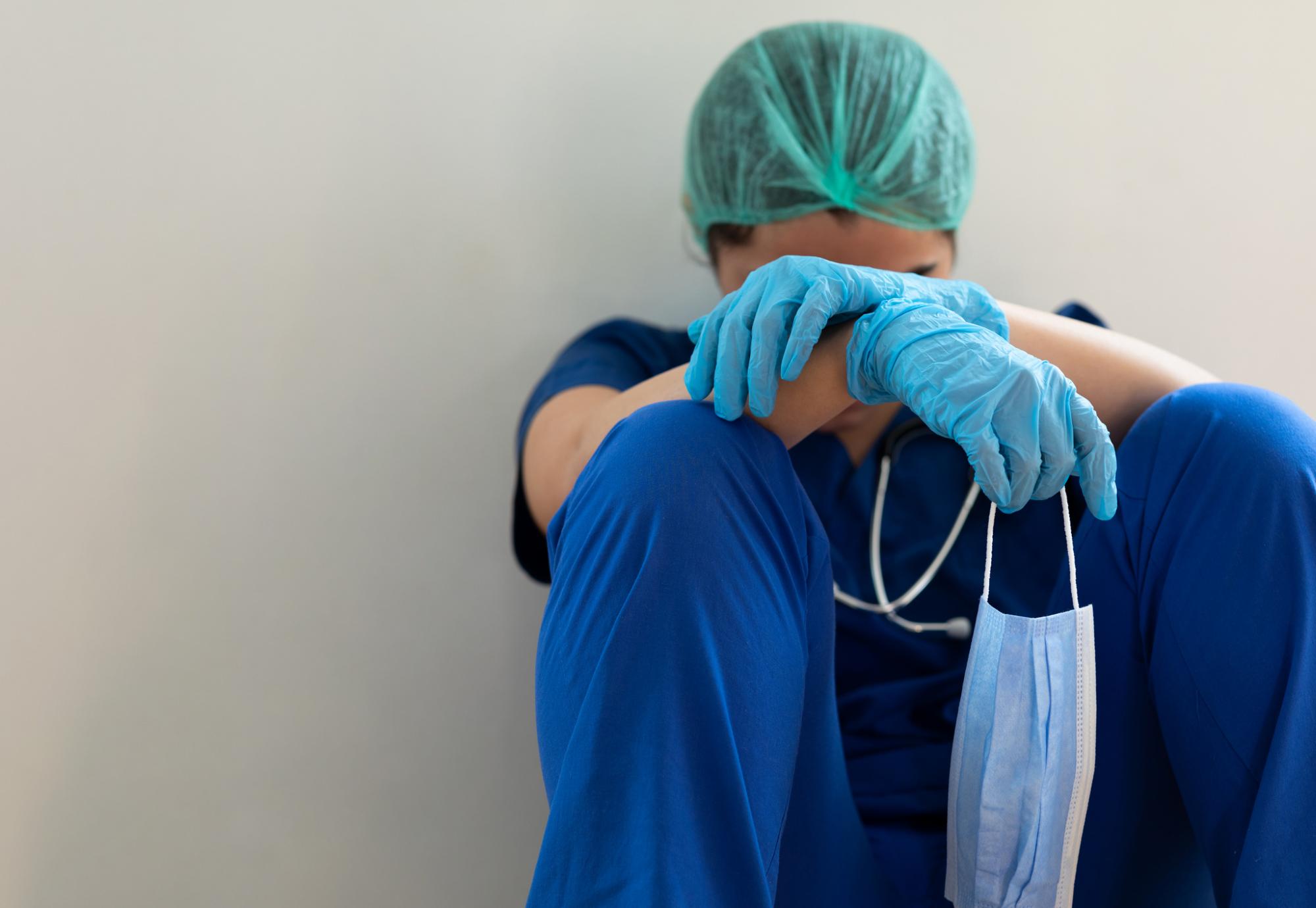
- Staff experienced widespread burnout, trauma and symptoms consistent with PTSD
The report highlights “intolerable” pressure on services that continued wave after wave, affecting emergency care, general practice, mental health services, maternity care and community health teams.
The report identifies multiple systemic failures, including:
1. Flawed early infection prevention and control guidance
Initial guidance assumed Covid‑19 spread primarily through surface contact, failing to account for aerosol transmission, which left staff and patients exposed.
2. Severe PPE shortages
Healthcare workers “sometimes worked in inadequate and unsuitable PPE”, putting themselves and their families at risk.
3. 111 services unable to meet demand
Call volumes surged dramatically, particularly early in the pandemic, leaving 111 unable to cope.
4. Ambulance delays and life‑threatening waits
Emergency ambulance response times worsened, even for the most critical cases, with some services requiring military assistance.
5. Devastating impact of visiting restrictions
Patients, including vulnerable individuals such as those with dementia, learning disabilities, children in mental health units and women in maternity care, were frequently left without vital support. Many died alone, a trauma that continues to devastate bereaved families.
6. Harmful public messaging
“Stay Home, Protect the NHS, Save Lives” may have unintentionally discouraged people from seeking urgent care, contributing to reduced attendances “even for life‑threatening emergencies such as heart attacks”.
The Inquiry details the heavy toll on NHS and care staff, with many experiencing post‑traumatic stress, suffering burnout, taking long‑term sickness absences, and feeling unsupported and unheard.
Witnesses included clinicians, frontline staff, policymakers, long Covid groups and bereaved families. In total, 95 witnesses gave oral evidence during Module 3 hearings.
Baroness Hallett calls for the prompt and full implementation of 10 recommendations to prevent future system collapse. These include:
- Expanding urgent and emergency care capacity, including surge capacity
- Strengthening infection prevention and control bodies and guidance
- Improving data collection, including better identification of high‑risk groups and accurate recording of healthcare worker deaths
- Standardising advance care planning
- Increasing support and retention programmes for healthcare workers
- Publishing clear guidance for clinical decision‑making if critical care resources become exhausted
Baroness Heather Hallett, Chair of the UK Covid-19 Inquiry, commented:
“This third UK Covid-19 Inquiry report concerns the impact of the pandemic on the UK's healthcare systems. I can summarise that impact as: we coped, but only just.
“The healthcare systems came close to collapse. Healthcare workers carried the burden of caring for the sick in unprecedented numbers. It came at a huge cost to them, their families, their patients and the loved ones of patients. Collapse was only narrowly avoided thanks to the extraordinary efforts of all those working in healthcare across the UK.
“Despite those efforts, some patients did not get the level of care they would usually receive. The enormous strain placed upon the healthcare systems was unprecedented. Those working within it were obliged to work under intolerable pressure for months on end.
“We cannot know when, but there will be another pandemic. My recommendations, taken as a whole, should mean that the UK is better prepared for that pandemic. In doing so, we shall avoid some of the terrible human cost of Covid-19. I urge governments across the UK to work individually and collectively to implement these recommendations, in full and in a timely manner.”

The Inquiry will monitor progress throughout its lifetime, with the next update due May 2026. Module 3 is the first to include a record from the Inquiry’s listening project, Every Story Matters, incorporating contributions from more than 32,000 people. The Healthcare Record reveals devastating accounts of loss, trauma and resilience.
The Inquiry’s next report – focused on Covid‑19 vaccine development and rollout (Module 4) – will be published on 16 April 2026, followed by further reports up to the final Module 10 report in Summer 2027.
Image credit: iStock