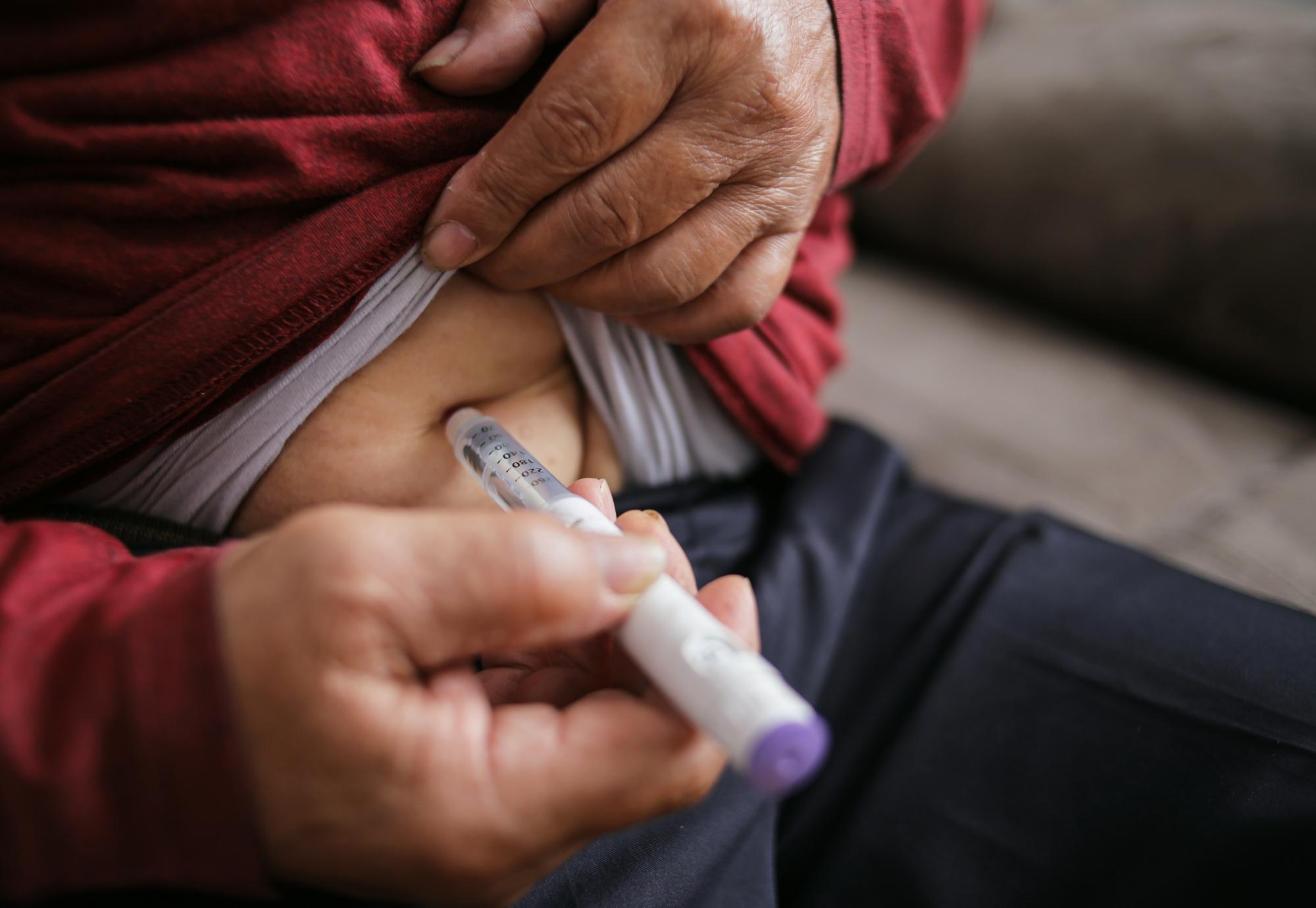
A new report from the Health Services Safety Investigations Body is calling for urgent action to improve access to specialist diabetes care for adults who self‑administer insulin and live with a mental health condition, warning that poor coordination between services is placing vulnerable patients at serious risk.
The investigation examined the experiences of patients supported by community mental health teams and found multiple incidents where people had intentionally not taken insulin as prescribed, including individuals with Type 1 Diabetes and Disordered Eating (T1DE). The report highlights several cases that resulted in life‑changing harm or death.
Stories shared by patients, families, carers and frontline staff revealed significant gaps in collaboration between mental health and specialist diabetes teams, despite the potentially fatal consequences of poor diabetes management.
The report identifies substantial issues affecting the safety and quality of care for people living with co‑existing mental health problems and insulin‑treated diabetes:
1. Patients Not Always Under Specialist Diabetes Care
Many people with diabetes and mental health needs are not being seen by specialist diabetes teams, even when their condition requires close monitoring.
2. Mental Health Teams Left Managing Diabetes Alone
Community mental health staff reported feeling responsible for diabetes management when patients had been discharged from diabetes services without reasonable adjustments for their mental health — for example, for people unable to leave their home due to anxiety.
3. Patients Disengaging Due to Stigma or Poor Communication
Some patients stopped attending diabetes appointments because they felt judged, criticised, or spoken to with “finger‑wagging” language. They described feeling misunderstood by services lacking awareness of their mental health circumstances.
4. Major Variation in Service Integration
Levels of collaboration between diabetes and mental health teams differ widely across the country, despite widespread recognition of the risks that poor integration poses to patient safety.
5. Homeless Patients Face Particular Barriers
People experiencing homelessness often struggle to access diabetes or mental health support due to service gaps, limited data and possible prejudice influencing resourcing decisions.
The report also highlights significant concerns about Type 1 Diabetes and Disordered Eating (T1DE), noting:
- A lack of consensus on what T1DE is
- Major research gaps around identification and treatment
- Severe risks of harm if not recognised early
Two powerful cases featured in the report — Alex and Megan, both of whom died — illustrate the life‑threatening nature of poor support and inadequate coordination. Their families shared their experiences to drive improvements in care.
Frontline professionals described patients with mental health conditions who have access to insulin as a “huge red flag”, with several staff reporting that they had known patients who died following self‑harm using insulin.
Community mental health teams also reported experiencing psychological harm and distress after incidents, underscoring the need for clearer pathways, training and joint working.
The report calls for stronger, more integrated relationships between specialist diabetes services, primary care and mental health providers. Its recommendations include:
- Improved service integration and shared care pathways
- Better recognition, understanding and research into T1DE
- More consistent national standards for collaborative working
- Adjustments to make diabetes care accessible for patients with mental health needs
- Better data and targeted support for people experiencing homelessness
Nick Woodier, HSSIB Senior Safety Investigator, said:
“Our report emphasises that too often individuals managing both diabetes and a mental health problem face a troubling disconnect between specialist physical and mental health services. This fragmentation of care can leave patients without the co-ordinated support they need, increasing the risk of harm. Alex and Megan’s cases demonstrate that these are not just abstract safety concerns documented in reports; they have a real and devastating impact on people and their families.
“The investigation also identified significant concerns around access to care, including the stigmatisation of mental health within the context of diabetes care, poor recognition of type 1 diabetes and disordered eating, and repeated failures to make reasonable adjustments for patients.
“Many of the issues we identified are long standing and persistent. Our recommendations are focused on reducing inequalities and removing barriers to care. We are calling for consistent, effective integration between diabetes and mental health services to deliver safer, more coordinated care and improved outcomes for people who are managing complex mental and physical health needs.”

The findings are intended to support safer, more person‑centred care for people living with both diabetes and mental health challenges, a group at heightened risk who often fall between the gaps of the current system.
Image credit: iStock